
Innovative Specialty Pharmacy Solutions
The Premier Specialty Pharmacy Care & Growth Accelerator
Improving lives and elevating performance are at the heart of everything we do. As the first and largest company in the nation to integrate specialty pharmacies in the place that’s most helpful to patients — their hospitals — our programs and data platforms reduce costs, achieve better clinical outcomes and accelerate system-wide growth.





Innovative Specialty Pharmacy Solutions
The Premier Specialty Pharmacy Care & Growth Accelerator
Improving lives and elevating performance are at the heart of everything we do. As the first and largest company in the nation to integrate specialty pharmacies in the place that’s most helpful to patients — their hospitals — our programs and data platforms reduce costs, achieve better clinical outcomes and accelerate system-wide growth.




More Impact With Lower Total Medical Expense
Learn firsthand how integrated specialty pharmacies can improve lives and reduce costs.

Financial Toxicity in Cancer Care
Financial toxicity, or the socioeconomic hardships caused by the cost of care, is a stark reminder of disparities in health care. Learn how an integrated health system specialty pharmacy can alleviate the burden for patients.

Kathy's Story: Finding Success in our Diabetes Care Coach Program
After 25 years of struggling to manage her diabetes, Kathy shares how the Diabetes Care Coach Program helped her take control of her health and dramatically lower her HbA1c levels.
The Shields Care Continuum
Achieving Quality Outcomes
Discover how our integrated and comprehensive offerings improve therapy management and care coordination for patients with chronic and complex diseases.

Nearly 1 million people in the U.S. live with Multiple Sclerosis. Our care model assists patients in achieving lower annualized relapse rates.
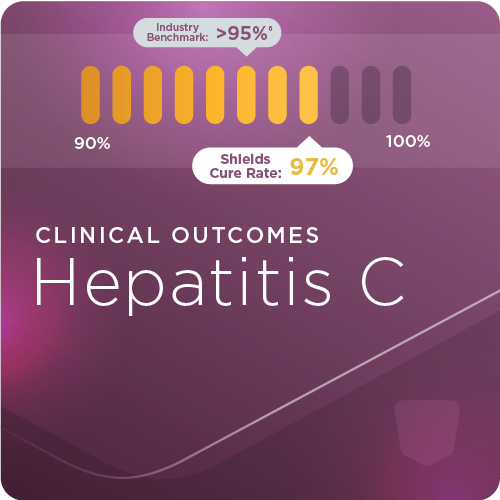
Shields Health Solutions can help patients with Hepatitis C prevent disease progression and achieve sustained viral response.
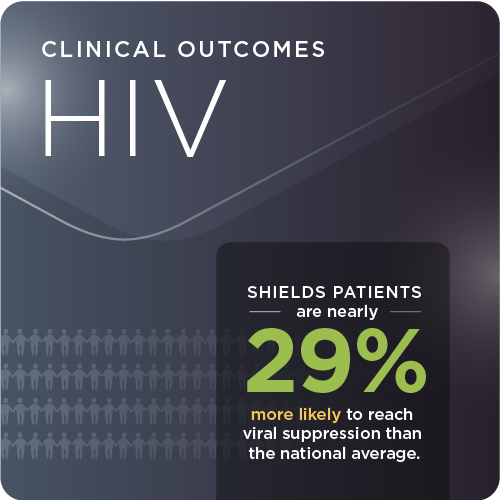
In the U.S., nearly 1.2 million patients living with HIV. Shields can help patients with access to our care model maintain viral suppression.

Our collaborative care model helps providers monitor this physically debilitating disease, which is vital to slowing progression.
Why Working With Shields is a Win-Win
One of our earliest partners, Baystate Health has been part of the Shields nationwide network of health systems for nearly a decade. Hear why their Chief Financial Officer feels that working with us is a win for patients, a win for physicians, and a win for his health system.


Trusted by Health System Leaders Nationwide
We work alongside health system leaders to improve lives and elevate performance where it matters most.





Trusted by Health Systems Nationwide
We work alongside health system leaders to improve lives and elevate performance where it matters most.




Collaborate With Us
Tell us about yourself and we'll connect you with the right team member.






